Obesity costs UK ‘more than violence and terrorism’ – study
Published 20 Nov, 2014 14:39 | Updated 21 Nov, 2014 10:08
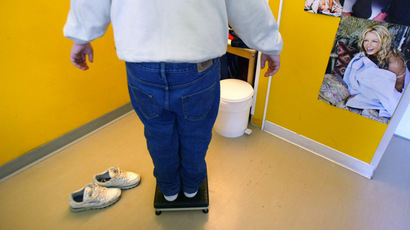
Obesity costs the UK more than armed violence, war and terrorism, a new study says. Research commissioned by McKinsey and Co found the UK loses 3 percent of its GDP treating obesity and related illnesses.
According to the McKinsey Global Institute (GMI), obesity has the second-largest health impact on the economy after smoking.
The UK currently spends £47 billion every year on the treatment of obesity, in comparison to armed violence, war and terrorism, which collectively cost the country £43 billion, or around 2.5 percent of GDP.
The study predicts by 2030 almost half of the world’s population would be overweight or obese, a figure which currently stands at 30 percent.
The GMI used the report to call for a “coordinated response” to the “global obesity crisis” by governments, retailers and the food and drink industry.
They propose a series of 44 measures for the UK which could collectively bring 20 percent of overweight Brits back to “normal” weight within five to 10 years, saving the UK around £16 billion, and the NHS £766 million, each year.
The report criticized the implementation of the UK’s response to the obesity crisis, saying their efforts were “too fragmented to be effective” and that the £638 million the UK spends on obesity programmes is “relatively low given the scale of the problem.”
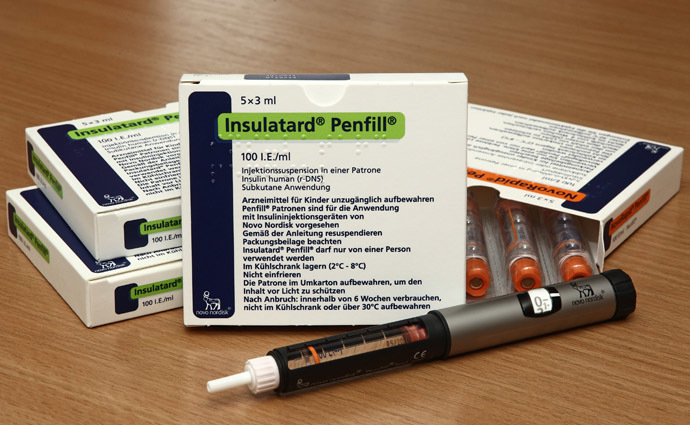
The cost of medical conditions related to obesity, however, was shown to be much higher. The UK spends £6 billion each year on obesity-related health problems, with a further £10 billion for diabetes treatment.
The report said “obesity is a major global economic problem caused by a multitude of factors. Today obesity is jostling with armed conflict and smoking in terms of having the greatest human-generated global economic impact.
“The global economic impact of obesity is increasing. The evidence suggests that the economic and societal impact of obesity is deep and lasting.”
This report follows claims from a National Bariatric Surgery investigation in November which claimed that young obese Brits would “cripple the NHS.”
During their investigation into 18,000 weight loss operations in the UK, the authors found that more young people were needing life-saving surgery, and that they were becoming more obese.
Of the total number of operations monitored, 550 were for patients under the age of 25, of whom 62 were under the age of 18.
Some 48 patients under 25 had a Body Mass Index (BMI) of 48.8 or more, and are classified as “super-obese.”
The Chief Nutritionist at Public Health England (PHE), Dr Alison Tedstone, said tackling the problem required communication between different sectors, both private and public.
“Overweight and obesity is a complex problem which requires action across individual and societal levels involving industry, national and local government and the voluntary sector,” she said.
“There is no single ‘silver bullet’ solution. Today 25 percent of the nation is obese and 37 percent is overweight. If we reduce obesity to 1993 levels, where 15 percent of the population were obese, we will avoid 5 million disease cases and save the NHS alone an additional £1.2 billion by 2034,” Tedstone said.