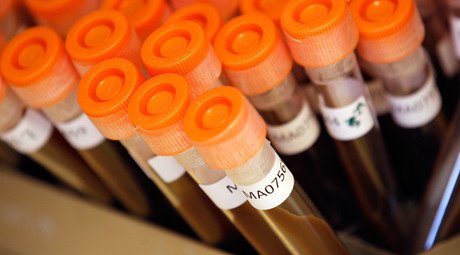
New arms race: Science versus antibiotic-resistant superbugs

The death rate from bacterial infections plummeted following the discovery of penicillin, but these microbes developed ways to resist our antibiotics. What threats do superbugs pose and what factors contribute to their emergence?
The discovery and development of antibiotics saved millions of lives during the latter half of the 20th century. Scottish bacteriologist Alexander Fleming, who witnessed soldiers with infected wounds perish while serving in the Royal Army Medical Corps during the First World War, per chance discovered a penicillin producing mold in 1928.
However, penicillin was not synthesized into medicinal form until over a decade later. Its subsequent mass production during the 1940s is credited with saving many lives during the Second World War.
WHO's 1st ever list of #AntibioticResistance priority pathogens.
— WHO (@WHO) February 27, 2017
New antibiotics to tackle them are urgently needed https://t.co/6SDXXjpXlI
Although penicillin’s use was initially restricted to military hospitals, it soon became accessible to the general public in industrialized nations. In 1946, penicillin first became available on prescription in the UK. People were jubilant over the discovery of a “wonder drug” that could cure many bacterial infections with high mortality rates, especially among infants and the elderly. For example, penicillin reduced the death rate of bacterial pneumonia from between 60-80 percent to 1-5 percent. Postoperative mortality rates also fell sharply.
However, reports of penicillin-resistant bacteria began to emerge only a few years later. The first penicillin-resistant strain of Staphylococcus aureus was identified in 1947. New penicillin-based antibiotics were duly manufactured, sparking an arms race between microbe and medicine.
In 1961, only a year after the antibiotic methicillin was introduced, the first case of Methicillin-resistant Staphylococcus aureus (MRSA) was detected in the UK. Today, MRSA is found in hospitals across Europe, the USA, and many other countries. Despite the development of newer antibiotics - presently there are over a 100 - which fight bacteria in myriad ways, the world’s oldest life forms have found ways to make our “wonder drugs” ineffective, such as mutating into drug-resistant forms or neutralizing the effects of the antibiotics.
In 2008 the US Centers for Disease Control and Prevention (CDC) reported that MRSA claims more lives than AIDS, with recent CDC estimates suggesting superbugs kill 23,000 Americans annually. A 2009 report published by the European Medicines Agency and the European Centre for Disease Prevention and Control (ECDC) estimated deaths attributable to some of the most common antibiotic-resistant bacteria and found that “the number of deaths attributable to infections due to the selected antibiotic-resistant bacteria in the EU, Iceland, and Norway was estimated at approximately 25,000 each year”.
This resulted in an additional €1.5 billion annually in “extra healthcare costs and productivity losses.” A 2014 report commissioned by the UK government projected that, if left unchecked, drug-resistant infections could kill 10 million a year globally by 2050 - more than cancer and diabetes combined - and cost $60 -100 trillion in lost economic output over the next 35 years.
It appears that despite our 21st-century technology, primitive unicellular organisms are getting an edge over us. But why are we losing ground in this battle? Several factors contribute to this state of affairs. First, the level of antibiotic use correlates strongly with the prevalence of antibiotic-resistant infections.
Both the UK government and NHS have in recent years launched campaigns against the inappropriate prescription of antibiotics. It was and still is, not uncommon for people to expect their GP to prescribe antibiotics for a sore throat or the common cold, which is caused by a virus and against which antibiotics are useless.
Last year, former UK Prime Minster David Cameron asked general practitioners (GPs) to halve the number of inappropriate antibiotic prescriptions - currently estimated to be 3.4 million a year - by 2020. There has been a similar crackdown against the overuse of antibiotics in hospitals, with their prescription being frequently audited. Increased awareness and more prudent prescribing have led to a recent reduction in antibiotic use within the UK.
However, healthcare is not the only case of widespread antibiotic usage. Antibiotics, as well as anti-fungals, are used in vast quantities in agriculture, namely food production, fish farming and crop growth. (It is reported that in the USA animals consume twice as many antibiotics as humans). Antibiotics are used prophylactically to prevent infections developing and spreading between animals that are farmed in confined conditions.
Until recently, they were also given to livestock to promote growth, though this practice was banned in Europe in 2006 and in the USA earlier this year. Animal consumption of antibiotics is expected to increase within emerging economies, such as the BRICS, over the coming years to match consumer demand. Just as increased human antibiotic use leads to greater bacterial resistance, the same is thought to be true when these drugs are used in agriculture, with drug-resistant pathogens being passed from animals to humans and having the potential to enter the food chain.
Producing newer antibiotics to match the emergence of novel strains of drug-resistant bacteria, as was previously the case, is not a straightforward affair.
Presently, pharmaceutical giants do not consider antibiotic development a priority, due to poor returns on their investments. Antibiotics are relatively cheap compared with other medicines and, together with their typically short duration of use and high cure rates, fail to generate the same profits as more expensive drugs that treat chronic illness. Furthermore, efforts to reduce antibiotic prescribing also adversely affects profit margins. An exception to the above is the development of antibiotics against MRSA, due to its worldwide prevalence.
Despite our advancements in science and medicine, we remain vulnerable to evolution’s earliest lifeforms. As the human and economic cost of antibiotic resistance is set to rise over the next few decades, political will, further investment in research and development, and a more judicious use of antibiotics is required if we are to successfully confront our ancient and invisible enemy.
Perhaps when the cost is sufficiently high, governments will be pushed to act and big pharma may see an opportunity for profit.
The statements, views and opinions expressed in this column are solely those of the author and do not necessarily represent those of RT.