Antibiotics 'fail 15%' of patients due to superbugs and ‘reckless’ prescription
Published 26 Sep, 2014 13:18 | Updated 26 Sep, 2014 13:19
One in seven patients can no longer be helped by antibiotics because they are increasingly ineffective after being handed out too freely by GPs. Experts warn that common infections could become potentially life-threatening for Britons.
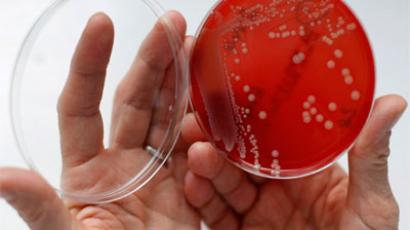
Researchers at the University of Cardiff say that GPs often prescribe antibiotics too readily, sometimes for viruses such as coughs and colds, for which antibiotics are ineffective, resulting in bacteria evolving into “superbugs” that are resistant to treatments that used to kill them.
An analysis of medical records showed that almost 11 million patients were prescribed antibiotics between 1991 and 2012 for sinusitis, sore throats, skin infections, bronchitis and pneumonia. Figures show overall antibiotic treatment failures increased from 13.9 percent in 1991 to 15.4 percent in 2012 – a rise of 12 percent.
Scientists said the findings were “bleak,” with one in six courses of antibiotics failing in 2012 – while for some drugs this was more than half.
The figures showed that potentially life-threatening pneumonia and bronchitis were the most resilient infections to treat, showing an increased antibiotics failure rate of 35 percent.
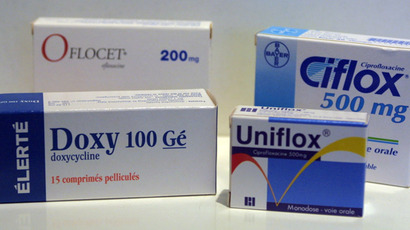
One antibiotic, trimethoprim, used to treat, for example, tonsilitis, failed up to 70 percent of the time when used to treat bronchitis or pneumonia. Another drug, the commonly prescribed amoxicillin, failed 18 percent of the time.
Professor Craig Currie, of Cardiff University’s School of Medicine, said: “The growing ineffectiveness of antibiotics is very worrying. We need to minimise unnecessary or inappropriate treatment which could be fuelling microbial resistance to antibiotics, prolonging illness and in some cases killing people.
“People are given antibiotics inappropriately. We can’t always test whether it’s due to a virus or bug, so antibiotics are a fallback.”
"There is a strong link between the rise in antibiotic treatment failure and an increase in prescriptions," Currie added. "Between 2000 and 2012, the proportion of infections being treated with antibiotics rose from 60 percent to 65 percent, which is the period in which we see the biggest increase in antibiotic failure rates."
England's chief medical officer, Sally Davies, in July last year warned the problem was so severe that routine hip operations, caesarean sections and even minor scratches could become deadly. She said resistance to antibiotics was one of the greatest threats to modern health. "If we don't take action, then we may all be back in an almost 19th century environment where infections kill us as a result of routine operations,” she said.
The problem of ineffective antibiotics has been declared a public health crisis by the World Health Organisation.
In April this year, the WHO already warned that once treatable common illnesses could become deadly because of the emergence of superbugs and the ineffectiveness of antibiotics. MRSA, one of the best known superbugs, is estimated to kill 19,000 people every year in the US and a similar number in Europe.
“The world is headed for a post-antibiotic era, in which common infections and minor injuries which have been treatable for decades can once again kill,” said Keiji Fukuda, the WHO's assistant director-general for health security.
In July, Prime Minister David Cameron said that resistance to antibiotics was a "very real and worrying threat," warning that Britain could be cast back “into the dark ages of medicine” if nothing is done.