Over 14 million low-income older Americans are food insecure - gov’t report
Published 15 Jun, 2015 23:25 | Updated 15 Jun, 2015 23:25
Some 17 million elderly Americans are in need of government-funded meal services, but 90 percent of them don't receive it, according to a new report by the Government Accountability Office. About 83 percent of those adults in need are food insecure.
“An estimated 90 percent of low-income older adults do not receive meals services like those funded by Title III programs, according to our analysis of 2013 CPS data,” the GAO wrote in a report released Monday. “About 83 percent do not receive meals among low-income adults who are food insecure, meaning they report three or more conditions such as skipping meals because they did not have enough money for food.”
The GAO analyzed the most recent data from two national surveys, the 2013 Current Population Survey (CPS) and the 2012 Health and Retirement Study (HRS). The report, requested by Sen. Bernie Sanders (I-Vermont), updated the agency’s findings from a 2011 report on what is known about older Americans’ need for services that were provided for by the Older Americans Act.
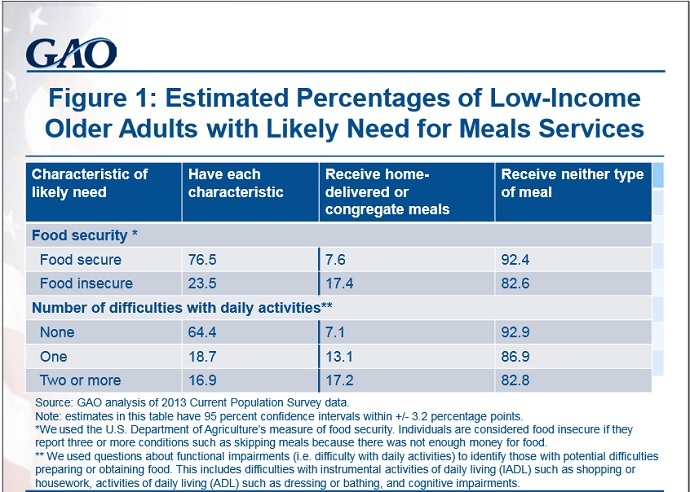
Comparing the data to a previous analysis using 2008 data, the GAO found that more low-income older adults were food insecure in 2013 (24 percent) than in 2008 (19 percent), even though “a substantially larger percentage of this population are receiving meals services (11 percent in 2008 compared to 17 percent in 2013).”
The Older Americans Act was signed into law by President Lyndon B. Johnson in 1965 to help older adults remain in their homes and communities. It created the Administration on Aging, as well as grant programs to help states care for older residents, including providing meals, transportation and assistance at home, according to the US Department of Health and Human Services (HHS).
The Older Americans Act was last reauthorized in 2006, and expired in 2011. Sanders called for the reauthorization of the legislation on Monday.
“A nation is judged by how it cares for its most vulnerable including the elderly and children. It is not acceptable that millions of elderly in this country are living in poverty and struggling to feed themselves,” Sanders said in a statement. “Instead of giving tax breaks to billionaires we should be expanding nutrition programs and other services for seniors.”
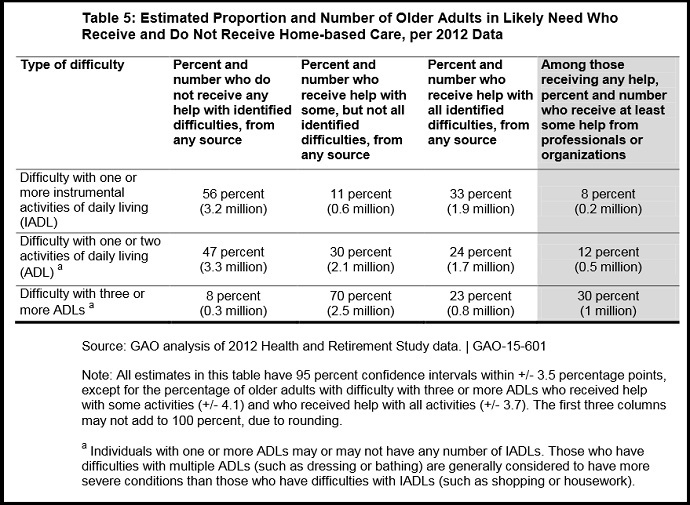
About one-fifth of retirement-age Americans ‒ meaning those 65 and older ‒ potentially need transportation services provided for in the Older Americans Act, similar to the percentage found in 2008.
“Then, as now, the extent of unmet transportation need is unknown among the population that may need it,” the GAO wrote. “In 2011, we recommended that the Secretary of Health and Human Services partner with others to develop uniform data collection procedures for obtaining information on older adults with unmet needs. The agency said it would explore options to implement this recommendation, though it has not fully implemented the recommendation to date.”
In March, Sanders and 32 other senators called on the Senate Appropriations Committee to increase funding in fiscal year 2016 for the programs created under the Older Americans Act by at least 12 percent over the fiscal year 2015 levels, or $225 million more.
“The demand for these programs is great, and in many areas of the country, vulnerable seniors are on waiting lists for services that they desperately need,” Sanders wrote in a letter to the chair and ranking member of the Senate Appropriations Committee. “Meanwhile, the cost of living continues to increase for seniors, particularly for food, medication, fuel and housing. Moreover, the demand is only expected to increase."
The letter was signed by the other 32 senators, including Angus King, an independent from Maine who ‒ like Sanders ‒ caucuses with the Democrats. No Republican senators signed the letter.
Hunger Free Vermont, a nonprofit organization that seeks to prevent hunger and promote good nutrition in the state, believes that Older Americans Act programs are a worthy investment.
“The OAA nutrition programs, including home delivered meals and congregate meals in senior centers, have been shown to be very effective in fighting hunger and keeping seniors healthy, out of the hospital, and living independently in their homes,” the group wrote in a statement celebrating Older Americans Month in May. “Investing in nutrition programs is cost effective; for the cost of an average hospital stay for a senior, that same person could get home-delivered meals for about five years.”














