New antibiotic found in ‘grassy field’ proves effective against drug-resistant bacteria
Published 8 Jan, 2015 23:20 | Updated 9 Jan, 2015 03:15
Researchers may have found a new antibiotic that bacteria will not become resistant to for decades, according to a new study. The discovery came not in a lab, but in soil from Maine, using a little-known device that’s “generating excitement.”
Dr. Kim Lewis, director of Northeastern University’s Antimicrobial Discovery Center, sought to find a new source of antibiotics other than synthesizing them in a lab. So he and Slava Epstein, a biology professor at the same Boston, Massachusetts school, headed into “a grassy field in Maine,” Lewis told reporters during a Tuesday conference call. They took a soil sample, which yielded teixobactin, the previously undiscovered antibiotic. The journal Nature published their research on Wednesday.
READ MORE:Scientists target 'universal' protein to treat brain cancer and Ebola
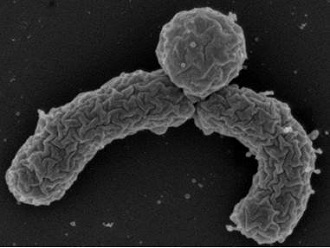
Lewis then tested the compound for resistance development and did not find mutant MSRA (methicillin-resistant Staphylococcus aureus) or Mycobacterium tuberculosis resistant to teixobactin, which was found to block several different targets in the cell wall synthesis pathway. The antibiotic was effective against the deadly ‒ and difficult to treat ‒ staph infection in mice as well.
Teixobactin is thought to attack microbes by binding to fatty lipids that make up the bacterial cell wall, and it is difficult for a bacterium to alter such fundamental building blocks of the cell, Nature reported. By comparison, most antibiotics target proteins and it can be relatively easy for a microbe to become resistant to those drugs by accumulating mutations that alter the target protein’s shape.
“Our impression is that nature produced a compound that evolved to be free of resistance,” Lewis said to news@Northeastern. “This challenges the dogma that we’ve operated under that bacteria will always develop resistance. Well, maybe not in this case.”
The antibiotic could be a huge weapon in the fight against drug resistance, a “serious threat” to world health. In the United States alone, at least two million people become infected with bacteria that are resistant to antibiotics each year, and at least 23,000 people die annually as a direct result of these infections, according to the Centers for Disease Control and Prevention (CDC).
“The world is headed for a post-antibiotic era, in which common infections and minor injuries which have been treatable for decades can once again kill,” Keiji Fukuda, the World Health Organization's assistant director-general for health security, said in April.

But teixobactin is also remarkable because it is 'uncultured,' meaning that standard laboratory culture techniques are not able to grow it, Dr. Jordan Betz, a bioengineer at the National Institute of Standards and Technology told RT.
“Case in point: something like 97 percent of the human gut microbes are unculturable at present,” he noted.
Researchers grew single cells from the soil sample in their natural environment, where they then divided and multiplied into colonies. Once the colonies formed, the bacteria were “domesticated,” and the scientists could collect them and start growing them in petri dishes in the laboratory, The New York Times reported.
READ MORE:A little bit of fat goes a long way to fighting staph infections - study
“Essentially, we’re tricking the bacteria,” Lewis said during the teleconference.
To do this, the team used a piece of equipment that was first written about in 2010 but didn’t gain any prominence until Lewis’ article was published.
“Teixobactin isn’t even the most promising part of its own story. That honour falls on the iChip – the tool that the team used to discover the compound,” according to National Geographic. “Teixobactin is a fish; the iChip is the rod. Having the rod guarantees that we’ll get more fish—and we desperately need more.”

The device is now generating excitement because it has the potential to reveal further undiscovered antibiotics, Nature reported. It enables previously unculturable microbes to thrive in the lab, and so makes it easier to discover bacteria that naturally produce compounds deadly to other pathogens.
“The technology is very cool,” Gerard Wright, a biochemist at McMaster University in Hamilton, Ontario, Canada, who was not involved with the study, told Nature. “Nobody knew if these bacteria produced anything useful.”
The iChip works by sorting individual bacterial cells harvested from soil into single chambers. The device is then buried back in the ground. Several molecules in that environment are able to diffuse into the device, allowing the bacteria to thrive in a more natural setting than a petri dish. Typically, only about one percent of microbes in a soil sample are able to grow in the lab; the iChip expands that number to 50 percent, according to the researchers.
“The method has the potential to be truly transformative, giving us access to a much greater diversity of environmental bacteria than previously imagined,” Gautam Dantas from Washington University in St. Louis, Missouri told National Geographic.
READ MORE:Drug-resistant ‘superbug’ found in Rio de Janeiro Olympic waters
Teixobactin has not yet been tested on humans, so its safety and effectiveness are not known. Studies in people will not begin for about two years, Lewis noted. Those studies will take several years, so even if the drug passes all the required tests, it still will not be available for five or six years. If it is approved, he said, it will probably have to be injected – not taken by mouth.
Dr. William Schaffner, an infectious disease specialist at Vanderbilt University, called the research “ingenious,” but cautioned that its efficacy is not guaranteed.
“It’s at the test-tube and the mouse level, and mice are not men or women, and so moving beyond that is a large step, and many compounds have failed,” he told the Times.
Lewis and Epstein co-authored the paper with colleagues from the University of Bonn in Germany, NovoBiotic Pharmaceuticals in Cambridge, Massachusetts, and Selcia Limited in the United Kingdom.









