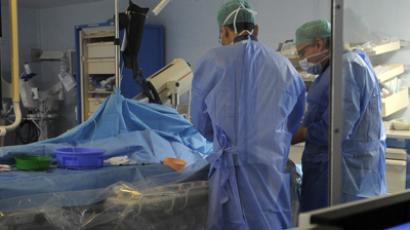
Workaholics: Mentally ill UK doctors forgo treatment
Published 7 Nov, 2012 11:24 | Updated 7 Nov, 2012 16:24
Thousands of practicing doctors in the UK have drinking problems and suffer from depression, several recent studies reported. They continue to treat patients because of a “culture of invincibility” and “presenteeism,” as well as a fear of exposure.
A GMC report found that 98 percent of 1,384 doctors who had underlying health concerns over the past five years were diagnosed with alcohol and substance abuse, or mental health issues. While there is no evidence to suggest that ill doctors have harmed patients in their care, the study argued it is likely that they provide a “less good service.”The Practitioner Health Program (PHP), a new service that doctors can contact to seek heath advice, found that out of 554 referrals, 28 percent were related to substance addiction and 85 percent were connected to mental health issues.Dr. Max Henderson from King’s College London’s Institute for Psychiatry believes that these figures are the sign of a much more widespread problem. A recent study carried out by Dr. Henderson found that doctors are often shamed out of saying they are sick or need extra time off.“Doctors feel ashamed of being unwell and they don’t deal with illness well, they find it hard to exchange the doctor role for the patient role,” Dr. Henderson explained to RT.“Doctors are often concerned about confidentiality or that colleagues or patients may stigmatize them for being unwell,” he said. “Given the social nature of the medical profession, doctors can find normal paths of treatment closed to them, so they tend to treat themselves or get corridor consultations.”Dr. Henderson explained that the PHP has been a very successful program since it was first introduced in London. Doctors who were ‘very unwell’ when they first came returned to work after treatment at rates of 70 to 80 percent. Dr. Henderson stressed that it is important for doctors to have access to trustworthy services like the PHP. Health problems among medical practitioners are often attributed to burnout from the stress and pressures of work. The Independent talked about the subject with Dr. Peter Verow, a respected consultant who represented the UK at squash in the Olympics. At the age of 55, he was suddenly hit by depression and went from exercising daily to not being able to get out of bed. Dr. Verow said he refused to admit his problems, and continued to go to work despite suffering from severe depression. “I was probably ill for six months to a year before I finally accepted I had to go off work,” he said. After seeing a psychiatrist, Dr. Verow took six months off. “My time away helped me to recognize that I had to change my work role in some way and so I went part-time,” he said. Dr. Henderson, along with the Royal College of General Practitioners, called this past weekend for more funding for support services for doctors, and warned that cuts and reforms to Britain’s National Health Service would only compound the problem.Dr. Henderson explained that virtually all doctors have no problem “dealing with daily exposure to blood, death, pain and sadness,” but that recent NHS reforms have damaged morale for many physicians. Though they work fewer hours, the traditional team structure of the work environment is gone, and the camaraderie and support along with it – junior doctors now often work with a different consultant every week. Cuts to non-essential staff like receptionists have also resulted in an increased workload for doctors. Dr. Clare Gerada, PHP's medical director and chair of the royal college, said that they are witnessing more sick doctors – GPs in particular – more shame and more presenteeism as doctors worry about their futures.