Last line breached? Deadly gene resisting all forms of antibiotics found in China
Published 19 Nov, 2015 12:07
Scientists have identified the first gene helping bacteria resist the only antibiotic group known to be effective when all others fail. Chinese and British experts came to the alarming conclusion that our last line of antibiotic defense has been breached.
The conclusion follows a large body of prior research that warns humanity about the dangers of becoming completely resistant to antibiotics. Now, Chinese doctors cooperating with UK specialists from Bristol and Cardiff Universities say we could soon be looking at the spread of uncontrollable superbugs.
In the research published in the journal Lancet Infectious Diseases, the researchers predict a return to the Dark Ages, when even common germs like E. Coli put a person in mortal danger.
"These are extremely worryingly results," professor and co-author on the study Liu Jian-Hua, from China’s Southern Agricultural University, said in a press release.
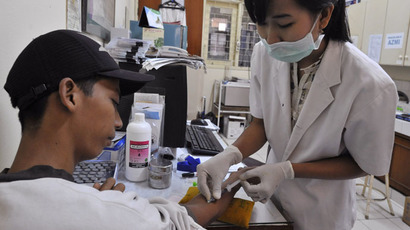
The research looked closely at Chinese farms, where it’s believed this dangerous potential for resistance took its root before spreading to humans.
'Invincible' bacteria threatens global epidemic: study https://t.co/DeenlBBEz6pic.twitter.com/Uwto2ohpUe
— Agence France-Presse (@AFP) November 19, 2015The culprit is the gene MCR-1, which allows common bacteria to develop resistance to polymixins, the antibiotic group considered our safest bet when fighting superbugs. The researchers detected it in the common, yet deadly, E. Coli and K. Pneumoniae, which cause pneumonia and blood disease. What’s more, the MCR-1 gene spreads easily from strain to strain, allowing a given bacteria to mutate faster than we can come up with solutions.
"The polymyxins (colistin and polymyxin B) were the last class of antibiotics in which resistance was incapable of spreading from cell to cell," the author explained further. "Until now, colistin resistance resulted from chromosomal mutations, making the resistance mechanism unstable and incapable of spreading to other bacteria.
"The emergence of MCR-1 heralds the breach of the last group of antibiotics," Liu continued. "Although currently confined to China, mcr-1 is likely to emulate other resistance genes ... and spread worldwide. There is a critical need to re-evaluate the use of polymyxins in animals and for very close international monitoring and surveillance of mcr-1 in human and veterinary medicine."
Use of antibiotics in cattle feed leads to airborne antibiotic-resistant bacteria – study http://t.co/OM3RU3Djogpic.twitter.com/D5LgZ0hmZg
— RT America (@RT_America) March 31, 2015The gene was discovered on plasmids – mobile versions of DNA which are more easily copied and transferred between different microbes. This is what worries the scientists, because it means the spread could be much more aggressive and can affect a more diverse range of bacteria.
"This is a worrying report, as polymyxins are often the last resort antibiotic to treat serious infections," Laura Piddock, professor of microbiology at the University of Birmingham, said, according to AFP. "Equally worrying is that this type of resistance can be easily transferred between bacteria." And according to Piddock, the spread could mirror other drug resistance mechanisms, such as that of tuberculosis.
Colistin is commonly used on Chinese farms, with pigs the prime contenders for hosting bacteria capable with the type of resistance associated with MCR-1. According to the researchers’ report, the samples containing the gene can be found in pigs, chickens and people in southern China, but that resistance originated in the animals.
The gene was actually discovered by accident, during routine farm testing on pigs and chickens. The researchers then took the E. Coli and K. Pneumoniae samples collected from the animals and matched them to the lab results they received from patients at two hospitals in the Guangdong and Zhejiang provinces. MCR-1 was found in over 20 percent of tested animals and in 16 of the 1,322 human samples.
The researchers say the lower infection rate among humans is proof they weren’t the first ones to cultivate the resistance.
"If MRC-1 becomes global, which is a case of when not if, and the gene aligns itself with other antibiotic resistance genes, which is inevitable, then we will have very likely reached the start of the post-antibiotic era," Professor Timothy Walsh of the University of Cardiff, who collaborated on the study, told the BBC News.
"At that point if a patient is seriously ill, say with E. Coli, then there is virtually nothing you can do."
Scientists on the research hope the study will serve to ignite the debate on the use of colistin in animal husbandry.
"The finding that this type of resistance can be shared by different bacteria - irrespective of whether from food, an animal or a person - is further evidence that the same drugs should not be used in veterinary and human medicine," said Piddock.
Further to that, according to Dr. Bruce Hirsch, infectious disease specialist at North Shore University Hospital in Manhasset, NY, doctors and patients should also understand the increasing responsibility to reduce antibiotic intake.
"If you don't need antibiotics, don't take them. You are only giving bacteria extra practice,” he was cited by HealthDay as saying.